TL;DR
Struggling to get breast reduction covered by UK private medical insurance? WeCovr, an experienced broker, explains how to prove medical necessity and navigate the cosmetic exclusion trap.
Key takeaways
- UK PMI policies exclude cosmetic surgery but may cover 'medically necessary' breast reduction.
- Success depends on proving significant physical symptoms like chronic pain, not aesthetic desires.
- A detailed GP referral and a supportive consultant's report are the most critical pieces of evidence.
- Insurers often require a stable BMI and evidence that conservative treatments have failed.
- If your claim is rejected, you have the right to appeal the decision with further evidence.
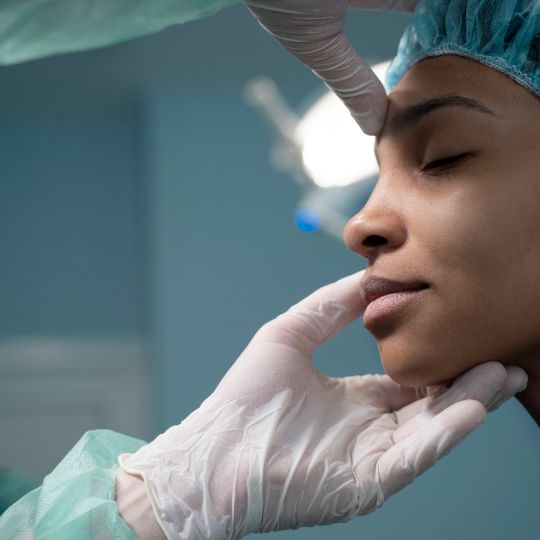
For thousands of women across the UK, the weight of their breasts is not a matter of appearance, but a source of chronic, debilitating physical pain. Yet, when they turn to their private medical insurance for help, they often hit a wall: the "cosmetic exclusion". At WeCovr, where our experienced team has helped arrange over 1,000,000 policies of various kinds, we understand this frustrating journey. This article is your definitive guide to navigating the complex world of UK private health cover to prove that a breast reduction is not a choice, but a medical necessity.
How to prove to your insurer that a procedure is causing physical pain, not aesthetic concern
Proving medical necessity for a breast reduction (reduction mammaplasty) hinges on one core principle: demonstrating, with robust evidence, that the procedure is intended to relieve clear physical symptoms, not to improve your appearance. Insurers are businesses, and their policies are contracts. Your task is to show them that your situation falls under the 'treatment for an acute medical condition' clause, not the 'cosmetic surgery' exclusion.
Success requires a methodical approach, shifting the narrative from "I don't like how my breasts look" to "My breasts are causing me significant, documented physical harm." The entire process, from your first GP visit to your pre-authorisation request, must be framed around function, not form.
Understanding the "Cosmetic Exclusion" in UK Private Medical Insurance
Nearly every private medical insurance policy in the UK contains a 'general exclusion' for cosmetic or aesthetic surgery. This is a fundamental principle of PMI.
Private medical insurance is designed to cover the diagnosis and treatment of acute medical conditions that arise after your policy begins.
An 'acute condition' is a disease, illness, or injury that is likely to respond quickly to treatment and lead to a recovery. Chronic conditions, which are long-term and have no known cure, are typically not covered.
Cosmetic surgery, in the eyes of an insurer, does not treat a medical condition; it alters appearance. However, there are crucial exceptions:
- Reconstructive Surgery: Surgery needed to restore function or appearance after an accident, cancer treatment (like a mastectomy), or major surgery.
- Medically Necessary Surgery: Procedures that, while they may alter appearance, are performed primarily to alleviate a documented medical problem that is causing physical symptoms.
A breast reduction can fall into this second category. The burden of proof, however, rests entirely on you, the policyholder, to convince the insurer that your case meets their strict criteria for medical necessity.
What is "Medically Necessary" Breast Reduction? The Insurer's Perspective
To an insurer, a "medically necessary" breast reduction is a treatment for a condition, often referred to as macromastia (the medical term for disproportionately large breasts). They are not interested in cup size or how you feel about your body image. They are interested in hard, clinical evidence of physical suffering.
Your case must be built around a collection of clear, recognised symptoms:
- Chronic Pain: Persistent and severe pain in the neck, upper back, and shoulders that is unresponsive to standard painkillers or physiotherapy.
- Postural Issues: Documented changes to your posture, such as a stoop or kyphosis (curving of the spine), directly attributable to the weight of your breasts.
- Nerve Pain/Compression: Symptoms like numbness or tingling in the arms or hands (brachial plexus compression) or nerve pain along the ribcage.
- Skin Conditions: Recurrent and difficult-to-treat skin infections, rashes, or cysts under the breasts (intertrigo) caused by skin-on-skin friction and trapped moisture.
- Permanent Grooving: Deep, painful, and often permanent indentations in the shoulders caused by bra straps digging into the skin.
- Interference with Daily Life: A documented inability to participate in normal physical activities, exercise, or sports due to pain, discomfort, or the sheer physical obstruction of large breasts.
Insider Tip: While the psychological distress caused by these symptoms is very real and should be mentioned, it should typically be presented as a consequence of the physical pain, not the primary motivation for the surgery. Frame it as: "The constant back pain and inability to exercise has led to feelings of depression," not "I feel depressed about my breast size."
Your Step-by-Step Guide to Building a Watertight Case for Your Insurer
A successful claim is not a matter of luck; it's a matter of meticulous preparation. Follow these steps to build the strongest possible case for pre-authorisation.
Step 1: The Crucial GP Consultation
Your journey begins at your GP's surgery. This is not a conversation to have on the fly; you should consider whether you may need to go prepared.
- Book a dedicated appointment: Tell the receptionist you may need to discuss a long-standing musculoskeletal issue.
- Focus exclusively on physical symptoms: Use the list above. Talk about the back pain, the skin rashes, the shoulder grooves, the inability to run or exercise.
- Detail what you've already tried: Explain the different types of supportive bras you've purchased, the painkillers you've taken, and any physiotherapy or osteopathy you've undergone. This demonstrates you have already attempted "conservative management."
- Keep a symptom diary: For a few weeks before your appointment, keep a simple diary rating your pain (1-10) and noting how it impacts your daily activities. Bring this with you.
- Request a specific referral: Ask your GP for a referral to a consultant plastic surgeon on your insurer's approved list to "assess the physical symptoms caused by macromastia for consideration of a functional reduction mammaplasty." The wording is key.
Your GP's referral letter is the first official piece of evidence. It must clearly document your physical complaints and the history of your condition.
Step 2: Gathering Your Evidence Portfolio
While you wait for your specialist appointment, build your file.
| Evidence Type | Description & Purpose |
|---|---|
| Symptom Diary | A dated log of your pain levels, symptoms (rashes, numbness), and how they limited your activities each day. This shows a chronic pattern of suffering. |
| Record of Failed Treatments | Keep receipts and records for specialist bras, physiotherapy sessions, chiropractor appointments, and prescriptions for pain or skin conditions. |
| Photographic Evidence | Take clear, non-sensational photos of the physical evidence: the deep grooves in your shoulders and the rashes or infections under your breasts. |
| Weight & BMI Stability | Insurers almost universally require a stable Body Mass Index (BMI), typically below 27-30, for at least 6-12 months. This is to help support the breast size isn't related to being overweight and that surgery outcomes will be stable. |
Expert Tip: Managing your BMI can be a challenge. As a WeCovr client, you get complimentary access to CalorieHero, our AI-powered calorie and nutrition tracking app. It's a fantastic tool to help you document a stable and healthy weight, strengthening your case for the insurer.
Step 3: The Specialist Consultant's Role
The report from your consultant plastic surgeon is the cornerstone of your claim. Your insurer places immense weight on their regulated, expert opinion.
During your consultation, the surgeon will:
- Take a detailed medical history, focusing on your symptoms.
- Perform a physical examination.
- Discuss the surgical procedure.
Crucially, their report back to your GP and the insurer must explicitly state:
- The diagnosis (e.g., symptomatic macromastia).
- That the primary reason for surgery is functional and medical, not aesthetic.
- A list of the physical symptoms the surgery aims to resolve.
- An estimate of the amount of tissue to be removed from each breast (in grams). A larger amount often strengthens the medical case.
Step 4: Submitting Your Claim & Seeking Pre-Authorisation
Before any procedure, you must get pre-authorisation from your insurer. This means they formally agree in writing to cover the costs.
- Contact your insurer's claims department: Inform them you are seeking pre-authorisation for a reduction mammaplasty. They will give you a claim number.
- Provide all information: You will need to provide the consultant's name, the hospital's name, the procedure code, and the estimated costs.
- Submit your entire evidence portfolio: Send the GP referral, the consultant's report, and any supporting evidence you have gathered. Make it as easy as possible for the case manager to see the full picture.
This is where having a specialist at WeCovr or one of our broker partners can be invaluable. We understand the claims process inside and out and can help help support your submission is clear, complete, and compelling, saving you stress and time.
Insurer-Specific Criteria: What Do Bupa, AXA, Aviva, and Vitality Look For?
While all major UK PMI providers follow the same core principles, their specific criteria can vary slightly. It is essential to read your policy documents. The table below provides a general guide based on industry practice.
| Insurer | Key Criteria (General Guide) | Typical Stance |
|---|---|---|
| Bupa | Often references the "Schnur Sliding Scale," a tool relating breast size to body surface area to determine medical necessity. Requires clear evidence of physical symptoms and failed conservative treatments. | Will consider cover if strict medical criteria are met and fully documented by a specialist. |
| AXA Health | Focuses heavily on the presence of significant physical symptoms (pain, skin issues). BMI must be stable and within a healthy range (often <30). The consultant's report is paramount. | Open to covering medically necessary procedures, but evidence must be irrefutable. Scrutinises the functional vs. aesthetic motivation. |
| Aviva | Requires a clear history of symptoms and documented attempts at non-surgical management like physiotherapy. A supportive GP and specialist are essential. BMI criteria are strictly enforced. | Follows a evidence-based approach. The claim will be approved if the medical case is strong and aligns with their policy wording. |
| Vitality | Known for their focus on wellness. They will want to see evidence that the condition is preventing an active lifestyle. BMI and a history of failed conservative treatments are key factors. | Will assess claims based on clear medical need. The link between the condition and a reduced ability to engage in healthy activities can be a strong point. |
Disclaimer: This table is for informational purposes only and is based on general industry knowledge. Criteria can change and are typically subject to the specific terms and conditions of your individual policy. check with your insurer directly.
The NHS Pathway vs. Private Insurance: A Comparison
It's helpful to understand the alternative. Getting a breast reduction on the NHS is possible but has become increasingly difficult.
| Feature | NHS Pathway | Private Medical Insurance Pathway |
|---|---|---|
| Eligibility | Extremely strict "exceptional circumstances" criteria. Varies by local Integrated Care Board (ICB). | Based on the terms of your policy and proving medical necessity to your insurer. |
| Waiting Times | Can be very long, often measured in years from referral to surgery, if you are approved at all. | Significantly faster. Once pre-authorisation is granted, surgery can often be scheduled within weeks. |
| Cost | Free at the point of use. | You pay your monthly premiums and any excess on your policy. The insurer covers the approved costs. |
| Choice | Limited choice of surgeon or hospital. | You can choose your consultant and hospital from your insurer's approved network. |
For those who can successfully prove medical necessity, PMI offers a much faster route to relieving debilitating symptoms.
What if Your Claim is Rejected? The Appeals Process
A rejection letter is disheartening, but it is not typically the final word.
- Request the Reason in Writing: The first step is to understand exactly why the claim was denied. Was it "insufficient evidence"? Was your BMI too high? Was the consultant's report not specific enough?
- Review Your Policy Document: Read the specific clauses they have cited. Check if their reasoning is consistent with the policy you paid for.
- Formulate a Written Appeal: Address the specific reasons for denial. If they need more evidence, provide it. You could ask your consultant to write a supplementary letter addressing the insurer's concerns directly.
- Gather More Evidence: Could you see a different specialist for a second opinion? Can you provide a longer symptom diary or more detailed records of failed treatments?
- Escalate to the Financial Ombudsman Service (FOS): If you have exhausted the insurer's internal appeals process and still believe you have been treated unfairly, you can take your case to the FOS. They will act as a regulated adjudicator.
Navigating a claims dispute can be complex. WeCovr specialists or broker partners often provides guidance to clients in this situation, helping them structure their appeal for the best chance of success.
Frequently Asked Questions
How much breast tissue needs to be removed for it to be considered medical?
Will my insurer cover a breast uplift (mastopexy) at the same time?
Do I need to have a certain BMI for my breast reduction to be approved?
Can I get cover if macromastia was a pre-existing problem?
Tackling the cosmetic exclusion trap requires persistence, evidence, and a clear strategy. By focusing on the functional and medical impact of your condition, you can transform your case from an aesthetic request into a compelling claim for necessary medical treatment.
WeCovr believes you shouldn't have to navigate this complex process alone. Whether you may need help understanding your current policy, fighting a claim, or finding a new PMI provider that suits your needs, our expert advisers are here to help. We can also provide discounts on other products like life insurance when you take out a health policy with us.
Ready to find clarity and get the support you deserve?
Sources
- NHS England
- National Institute for Health and Care Excellence (NICE)
- British Association of Plastic, Reconstructive and Aesthetic Surgeons (BAPRAS)
- Financial Conduct Authority (FCA)
- Financial Ombudsman Service (FOS)
- General Medical Council (GMC)
Important Information and Risks
No advice: This article is for general information only. It is not financial, legal, insurance, or tax advice, and it is not a personal recommendation. WeCovr does not assess your individual circumstances or recommend a specific product through this article.
Policy exclusions and underwriting: Insurance policies, including life insurance, private medical insurance, critical illness cover, and income protection, are subject to insurer underwriting, eligibility, acceptance criteria, terms, conditions, limits, and exclusions. Pre-existing medical conditions may be excluded, restricted, or accepted on special terms unless an insurer confirms otherwise in writing.
Tax treatment: References to tax treatment, HMRC rules, or business reliefs are based on current UK legislation and guidance, which can change. Tax treatment depends on your personal or business circumstances and may differ from examples in this article.
Before you buy: Always read the Insurance Product Information Document (IPID), policy summary, and full policy terms before buying, renewing, changing, or keeping cover. If you are unsure whether a policy is suitable for you, speak to an insurance adviser.
Start with your Protection Score, then decide whether private health cover is the right fit
Check where health access sits in your overall protection picture before deciding whether to compare private health cover.
Spot whether NHS access risk is the real issue
See if PMI is the gap to fix first
Get health insurance help only if it makes sense for you
Get your score
Start with your protection score
Check your current position first, then get health insurance help if you need it.
Check your current resilience
Score your income, health access and family protection position in a few minutes.
See where private cover helps
Understand whether faster diagnosis and treatment is a priority gap.
Continue to tailored PMI help
If health access is the issue, continue to tailored PMI help.
What you get
A quick view of your current protection position
A clearer idea of where the biggest gaps may be
A direct route to tailored help if you want it